
Caring for members
Delivering better health through the pharmacy benefit
We are dedicated to helping members stay adherent to the medications they need while tackling the pharmacy industry challenges that impact them – from the opioid epidemic to the quality, safety and cost effectiveness of their medication regimens.
Pharmacy solutions that make a difference
Polypharmacy
Simplifying complex therapies through collaboration
38 million working Americans are at-risk for complications due to overprescribed medications. That’s where the Optum Rx Polypharmacy Value Management Program can help. By targeting members taking five or more chronic medications, clients can expect to save an average of $850+ per successful intervention.1

Opioids
Addressing the epidemic with powerful results
Opioid misuse continues to be a national health care crisis. Nearly 9 million people misuse opioids in a year.3 The Optum Rx Opioid Risk Management offers a comprehensive solution for prevention, engagement, smart prescribing, and ongoing monitoring.
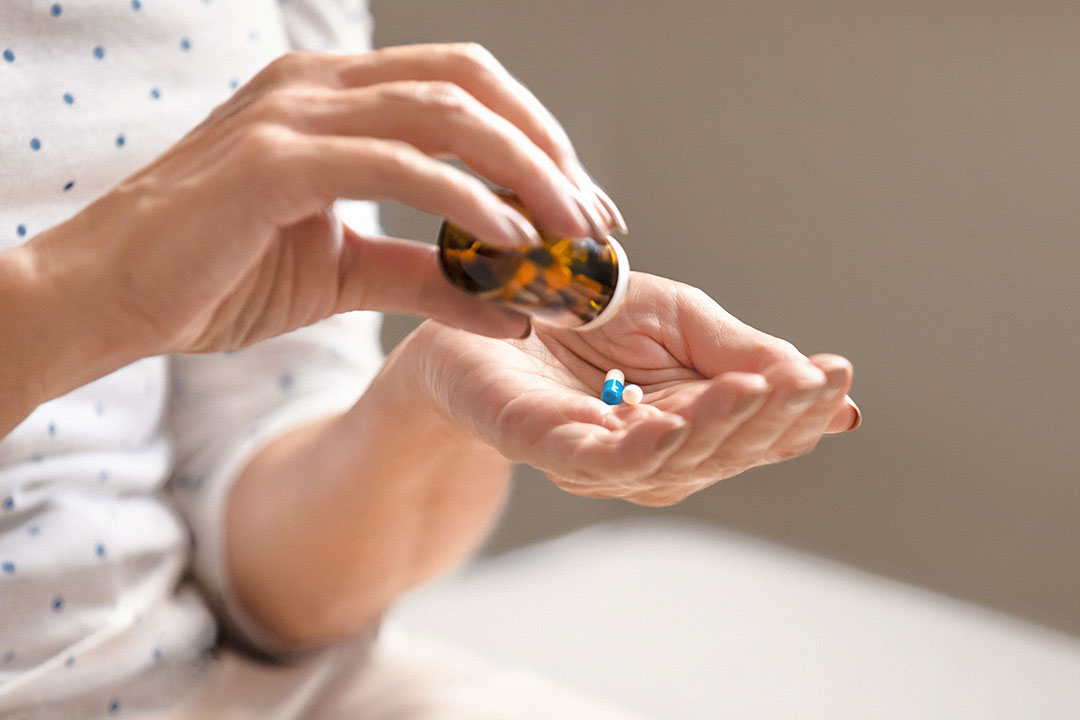
Helping members stay adherent
Better choices driven by a continuum of care
The Optum Rx Meds on Track program drives better clinical outcomes for members through a personalized, multi-channel care approach. From engagement to education and counseling, medication monitoring and gaps in care closure, we meet members where they are.

Fighting bad actors to save pharmacy costs
Our goal is to prevent, detect and correct fraud, waste and abuse
Every year, plan sponsors lose up to $300 billion in health care fraud, waste, and abuse.4 Optum Rx Audit Services run 24/7 behind-the-scenes at no cost to our clients. This latest case study shows how a union fund representing 8,800 lives realized more than $128,000 in savings and recoveries in one year.5

Multiple quality checks
Ensure orders are dispensed, packaged, and shipped safely
When it comes to prescription safety, triple checking is not enough. Our advanced automation combined with multiple safeguards and quality checks throughout the process helps ensure members receive the right medication with a 99.998% dispensing accuracy rate.6

Key benefits
Driving appropriate medication utilization helps control costs for both you and your employees.
Polypharmacy
$850+ plan savings per intervention of members taking five or more chronic medications.7
Award-winning Opioid Risk Management Program
Using our five-pronged approach, 97% of opioid claims are compliant with CDC guidelines.8
Meds on Track
48% of nonadherent members achieved PDC ≥ 80% after 6 months resulting in $26 per intervened member per month total cost savings.9
Fraud, waste and abuse
$184M in cost avoidance for our clients as a result of terminating 146 pharmacies due to suspected fraud findings.10
Pharmacist reviews
Multiple quality checks result in a 99.998% dispensing accuracy rate.11
Industry insights

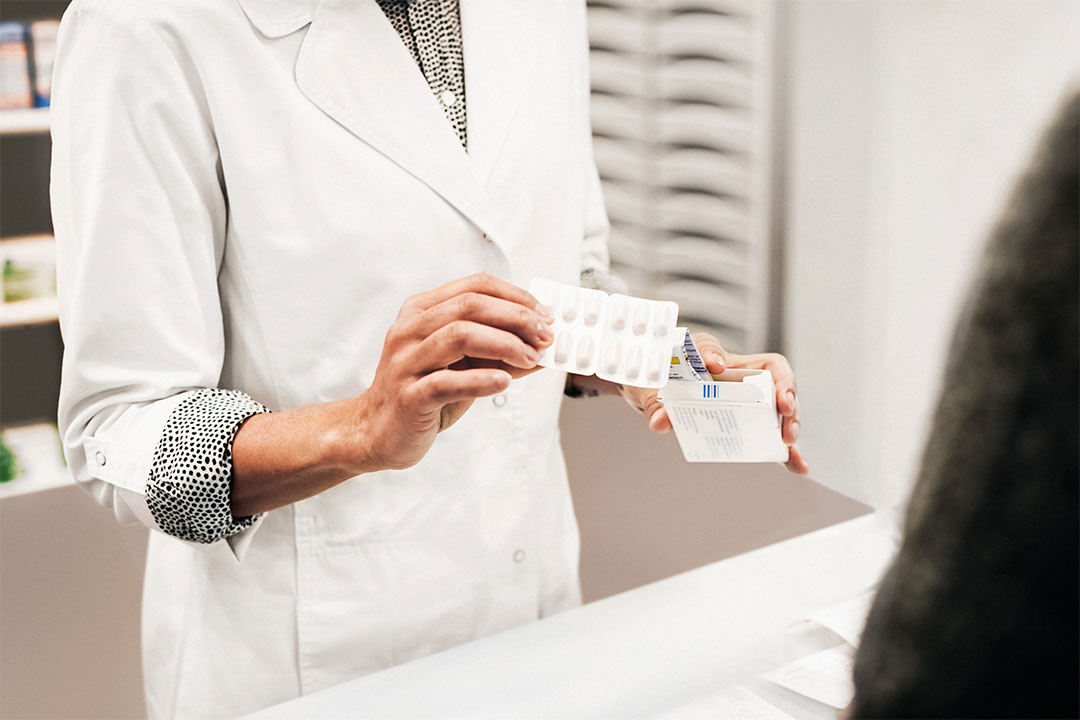
Article
Hear from a leader's perspective on how to manage polypharmacy.
![Fighting Fraud, Waste and Abuse in Pharmacy [Case Study]](/content/dam/optum-dam/images/business/insights/fighting-fraud-imagery-1080x720.jpg)
Case study
How one plan sponsor realized more than $128,000 in savings and recoveries in one year.
Complementary solutions
Driving appropriate utilization of medications
We are committed to helping members stay adherent to medications while addressing the industry challenges that prevent them from doing so.
Optum Rx Benefit Central™
Benefit Central is your cloud-based, self-service platform designed to streamline plan management — because your time is important.
Pharmacy benefits backed by data and insight
We help members, providers and clients act with clarity and confidence — earlier and faster.
- 2024 internal analysis.
- SAMHSA. Key Substance Use and Mental Health Indicators in the United States. 2021. Results from the 2020 National Survey on Drug Use and Health. Accessed April 20, 2022 at Key Substance Use and Mental Health Indicators in the United States: Results from the 2020 National Survey on Drug Use and Health (samhsa.gov)
- National Center for Drug Abuse Statistics. (2019). Opioid Crisis: Facts & Statistics on Prescription Opioid Addiction. NCDAS. https://drugabusestatistics.org/opioid-epidemic/.
- National Health Care Anti-Fraud Association. The Challenge of Health Care Fraud. Accessed May 30, 2025.
- Optum Rx. Internal analysis of recoveries under Standard Fraud, Waste and Abuse Audit Services. 2024.
- Optum home delivery book of business dispensing accuracy rate 2023.
- 2024 internal analysis.
- Percentage based on 2025 Optum Rx opioid metrics reporting.
- Optum Rx analysis. Metrics based on 1/14/2024 through 12/31/2024 Optum Rx internal non-Medicare lines of business utilization.
- Optum Rx analysis of book of business 2024 results
- Optum home delivery book of business dispensing accuracy rate 2024.

