Less friction, more confidence & better pharmacy experiences
Everyone uses their pharmacy benefits at some point. And too often, the experience is overly complicated. We’ve designed ours to work differently from the start. By connecting insight, technology and expertise across the pharmacy benefit, fewer things fall through the cracks. Clients and members benefit from a more predictable, coordinated experience powered by intelligence embedded directly into systems and workflows.
Guidance you can trust. Decisions you can stand behind. Outcomes that move healthcare forward for everyone.
Smarter decisions, powered by advanced analytics & expert guidance
Automation alone doesn’t build confidence. What matters is delivering the right insights at the right time so people can act on them.
Smarter plan management
Benefit plan builds in minutes
Optum Rx Benefit Central™ is your one-stop-shop for benefit management. Flexible configurations adapt to your needs, simplifying administration and accelerating turnaround times.
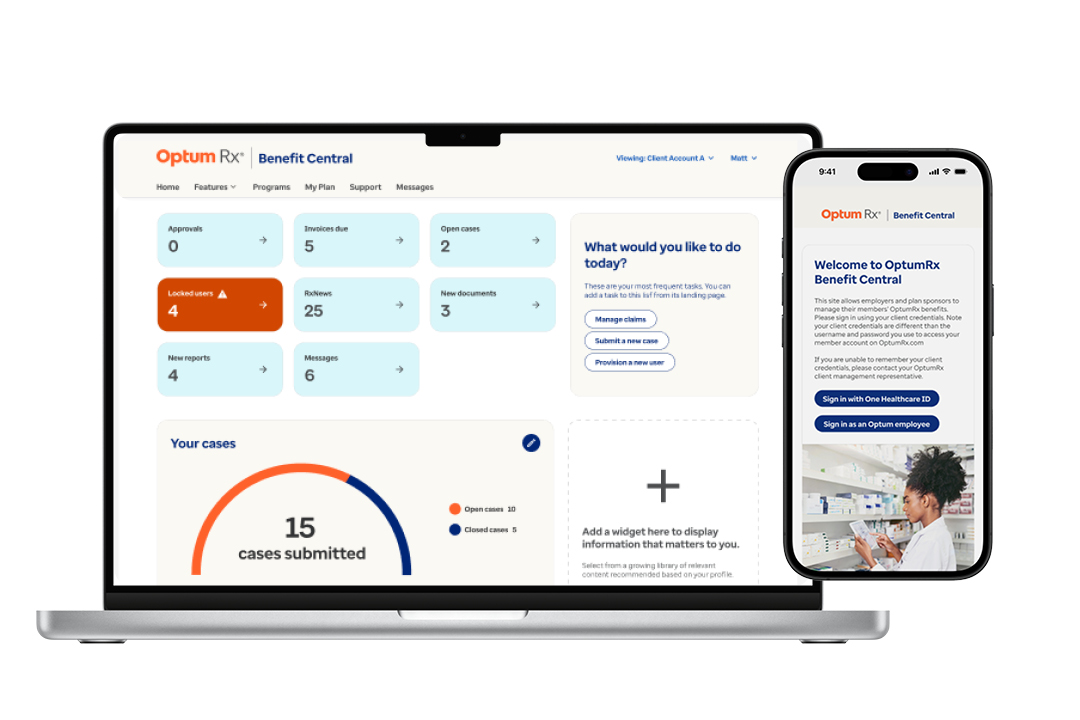
Faster decisions, fewer delays
Prior authorization approvals in under 30 seconds
Our industry-first innovation, PreCheck Prior Authorization expedites prior authorizations, decreasing turnaround times to under 30 seconds.1 With PreCheck MyScript®, members can save an average of $194, and clients save $393 per switched medication.2

Automated price visibility
Real-time cost savings for members
With MyScript Finder™, members can see medication cost information, including the lowest-cost option prior to their prescription being filled. Members who switch their medication save an average of over $90.
Price Edge automatically offers market-competitive medication pricing, saving members an average of over $60.2

Proactive risk management
AI-enabled fraud detection returns dollars to clients
Our AI-powered insights identify risk earlier, so teams can act sooner and prevent issues before they escalate. The result is $2M recovered per client on average in fraud, waste and abuse.2

A better member experience – built into every decision
We embed intelligence directly into the moments that matter, helping members access medications faster, avoid surprises and pay less without extra steps or delays.
Eliminating up to 25% of reauthorizations
We’re eliminating up to 25% of reauthorizations — more than 10% of overall pharmacy prior authorizations — to simplify access to prescription drugs.
Prior auth approvals in under 30 seconds
PreCheck Prior Authorization, an industry-first innovation, reduces the turnaround time to less than 30 seconds.1
Real-time prescribing details for doctors
PreCheck MyScript gives doctors real-time, plan-specific medication details at the point of prescribing, saving members $194 on average.2
Medication savings alerts for members
Proactive Savings Alerts identify savings opportunities and alert members directly, saving them $46 on average per 30-day script.3
Related healthcare insights

Article
Discover our latest innovation to the PA process — PreCheck Prior Authorization — which reduces approval times, appeals and denials.

Article
Two AI experts share insights on how we’re using AI and advanced technology to improve everything from trend prediction to member services.

White paper
Evolving federal policy on popular weight loss medications introduces additional cost and coverage uncertainties.
Complementary solutions
Driving appropriate utilization of medications
We are committed to helping members stay adherent to medications while addressing the industry challenges that prevent them from doing so.
Optum Rx Benefit Central™
Benefit Central is your cloud-based, self-service platform designed to streamline plan management — because your time is important.
- Optum Rx and Surescripts data. April - June 2024.
- 2025 analysis.
- PSA’s BOB for 2025.

