Every health plan approaches their payment integrity program with a unique set of capabilities, priorities and organizational structures. Regardless of the program's current design, a maturity assessment is essential for benchmarking progress across the maturity spectrum.
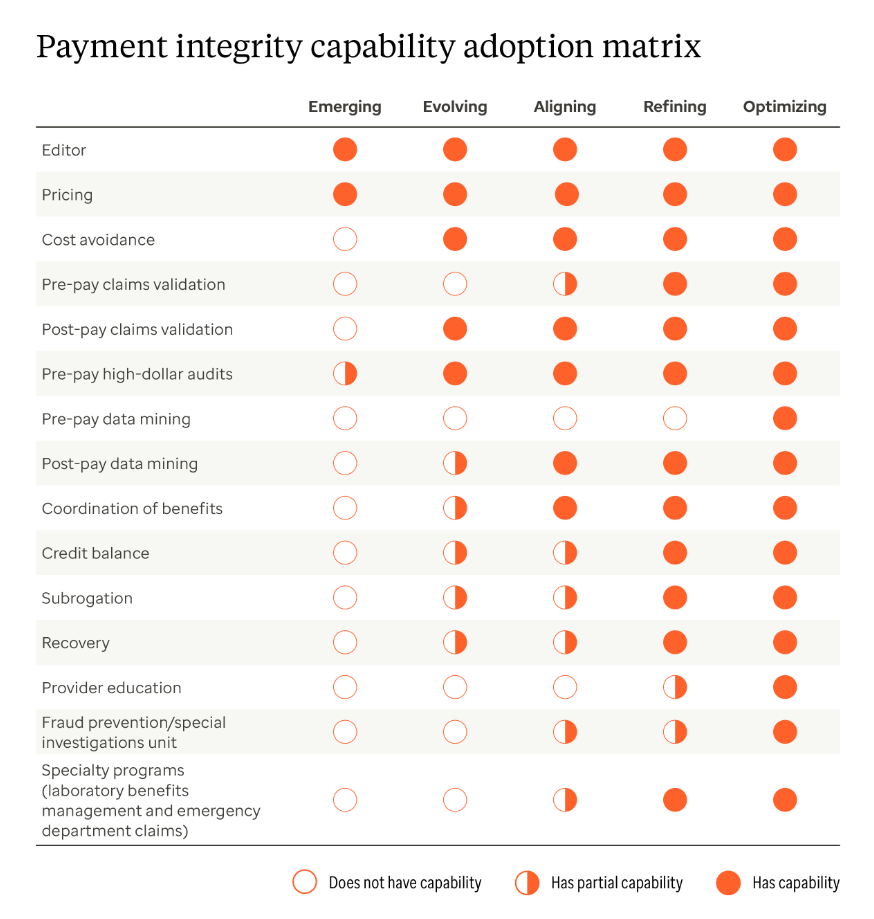
Optum defines payment integrity maturity across 5 levels:
- Emerging
- Evolving
- Aligning
- Refining
- Optimizing
By identifying exactly where they sit within these levels, health plans can move beyond their current state to bridge operational gaps, drive impact and build a strategic roadmap toward their long-term goals.



![5 AI Use Cases in Payment Integrity [White Paper]](/content/dam/optum-dam/images/business/insights/man-sitting-at-desk-using-computer-1080x720.jpg)