On-demand webinar
Visionary approaches to the OR
Watch experts reveal how leading health systems are using AI-enabled analytics to reduce surgical costs and improve operating room (OR) capacity.
Visionary Approaches to the OR
Good afternoon and welcome to today's program titled Visionary Approaches to the OR Tackling Cost and Capacity Challenges with Active Data Management. My name is Jay Asser, CEO, Editor for Health Leaders, and I'll serve as your moderator for today's program. Today's program is sponsored by Optum. Thank you to our sponsor and to you and our audience for giving us your time and attention. Before we get started, I have a few housekeeping details. 1st, to ensure that you can see all the content for the event, please maximize your event window and be sure to adjust your computer volume settings and or PC speakers for optimal sound quality.
Second, you will find a resources list for today's webinar on the lower right of your screen. Here we have listed materials from our sponsor for you to interact with. 3rd, at the bottom of your console are multiple widgets you can use. Should you experience any technical difficulties during today's program and need assistance, please click on the Help widget which has a question mark icon and covers common technical issues. We will have AQ and A portion at the end of the program. You may submit questions through the Q and A box in the lower left of the screen and Please note that all questions will remain anonymous.
Finally, it is my pleasure to introduce our speaker speakers for today's program. We have Laura Kennedy, Vice President of Client Success at Optum and Alex Warman, Administrator of Perio Operative Business Services at Lehigh Valley Health Network, part of Jefferson Health. Thank you both Laura and Alex for joining us today and taking the time to speak with us. The audience is yours. No, thank you. And and thank you to everyone for joining today. As Jay introduced us, we'll give a little bit more background, but as he said, I'm Laura Kennedy, I'm the Vice President of Client success, then Optum overseeing our value advisor teams across our provider technologies.
And so my teams are actually working side by side, perioperative leaders to ensure that they are getting the most value from the technology and are also providing strategic guidance and project support. I came to Optum from the Advisory Board back in 2017, but I've been collectively working in this space via the Advisory Board or Optum for almost 14 years, Alex. Thanks, Laura. Hello, everyone. I am Alex Warman. I am the administrator for Perry Op Business Services at Lehigh Valley, part of Jefferson. I've been with Lehigh Valley for 22 years.
I oversee perioperative business services over 14 surgical locations, focusing on data analytics, finance, operations and our scheduling and billing teams for our surgical practices across the system. Well, our presentation today is focused on the future. Hospitals and health systems are facing unprecedented challenges. Evergreen issues are further being compounded with net new supply and labor challenges that are only intensifying the pressures facing our operational leaders. So Alex and I want to really speak to the shift that progressive organizations are making to tackle cost and capacity challenges. And a huge part of that shift is centered on using robust analytics to achieve active data management.
So the majority of our time will be focused on best practices and real client stories from within our Crimson AIä cohort. But before we actually jump into the content, want to start off with a quick poll. So on the screen, you should see a poll that says, what's your most pressing issue keeping you up at night? We have staffing shortages and burnout, financial pressures and it's our third one. I can't read it. Inefficient scheduling, inefficient scheduling and supply chain disruptions and I'm sure everybody.
Yeah, go ahead, Laura. No, no, no, please, Alex. Yeah, I'm sure everybody's going to want to answer more than one of these, but we'll have to leave this screen on for you to select until we have enough answers. But please just pick the most pressing issue that you are encountering right now all. Right, we'll give it about another 20 seconds or so. All right, I'm not seeing any further dripping in. So let's go ahead and look at what you are saying is the biggest beast and no surprise here Alex, I, I'm looking at your smile and nod.
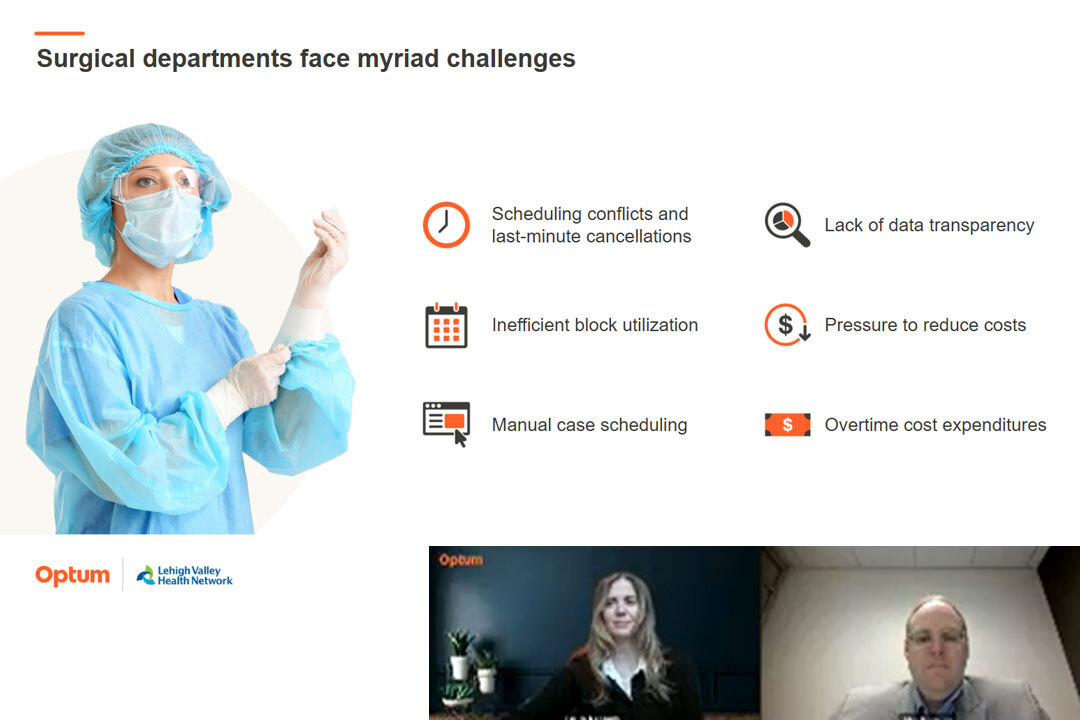
Yeah. It's, it's the pain point right now. I think we're all experiencing it and I think even the other items are probably just really just contributing to the financial pressures that we're all seeing. And we're more than glad to discuss that today in. Fact, there'll be a big portion of it. And so you know, no matter what you answered you can, you can't deny that the competing pressures are here. And so on the screen are some real life pain points from our multidisciplined perioperative leaders. You can read them. But Alex, I want to start with you.
Do you? Does any of this sound familiar? Oh, it it's, it's an everyday scenario. I mean, I, I get the call at seven O 5 in the morning. Hey, what what's going on with our volume for January? We're predicting low, how do we get more volume in, but how are we reducing our cost this month? We're over budget in our variance reporting. So it's coming in from all ends from our operational leaders, our physician chairs and even our high volume surgeons. So I think all of us are living this on a daily basis.
I know that to be true, but many on the line here I'm sure know all too well what that balancing act can be of appeasing your clinical leaders, your hospital administration and your surgeons, all while focusing on providing timely, good quality and cost effective care to as many patients as possible. And both the poll question and the issues on this screen really represent just a fraction of what perioperative departments are really facing. Cancellations, blocking efficiencies overtime, right? The list just goes on and on. You know, just think it took nearly a year to fully resolve the IV fluid shortage, yet all of you were having to find ways to meet patient and surgeon demands as if there was no disruption at all.
So with the growing patient waiting list, the staffing shortages, supply chain disruptions, optimizing your procedural areas has never been more critical. Alex, I like your thoughts on this as our perioperative leader here. Absolutely. And and you had to bring up the IV fluid shortage. You know, I mean that's still PTSD for most of us and even for some facilities they're still experiencing. But yes, I mean you, you see this list on the slide here at the scheduling conflicts, your inefficient block utilization, the manual case scheduling, the lack of data transparency and even the pressures to reduce costs and our overtime cost expenses.
Our operational leaders really want more volume, but we're we're all struggling with staffing shortages and burnout. Hospitals and surgical centers are grappling with a critical lack of skilled personnel and this is including surgeons, anesthesiologists, Crnas are Perry op nurses and scrub techs. Then on top of that, we have burnout, attrition, retirement, they're all exasperating the problem right now, especially in high volume centers. Are rising surgical volumes and even aging demographics and populations. Demand for surgical procedure is increasing due to our Asian demographics. It's due to chronic disease placing strain on already stretched surgical systems, financial pressures and reimbursement challenges.
We have inflation, rising anesthesia costs, declining reimbursement rates. We're squeezing our surgical departments. We're pushing more into AS CS, we're making it harder to maintain profitability and it's very hard to continue to invest in innovation and we have to enhance our OR utilization. Hospitals are focusing on maximizing operating room throughput. We need to reduce turnover and we need to improve. Case mix planning and our side of care work. So just a few. And unfortunately the hard is only getting that much harder right. So there's a lot of policy uncertainty.
You know there's funding cuts that have led to a reduction in reimbursement for some of our high margin elective procedures like a joint replacement, which are something that organizations really depend on to drive some of their profits. Economic volatility, rising costs, the reduced reimbursement rates, loss of insured patients, these are all putting creating a strain on financial sustainability and the burden of that is ultimately falling onto the hospitals themselves. The workforce pressures, you know, some hospitals, in fact probably many, their first form of action is to consider staff reductions to manage these costs. But you're risking long term operational capacity, especially in the surgical departments.
And in fact, there was a recent 2025 Advisory Board head of their 2025 nurse survey. And in that it actually highlighted that a pivotal challenge for the nursing workforce is that over 50% of bedside nurses are considering leaving direct patient care with few planning on returning. So Alex spoke to it anecdotally. We're seeing it in the data at a large scale and it's just going to continue to intensify. And then this last market factor, market force that's really making our lives a little bit harder here is strategic ambiguity. And I mean this in two ways.
1, you know, this is unprecedented times and so organizations are just really varying on how they want to tackle some of these broader issues. So some are pre active, proactive, others are reactive and there's no universal best practice on how you should attack some of these pressures. And the second point is around AI. So you see this here, you know, 90% of organizations are really investing in AI and looking to AI as a way to find some cost savings and efficiencies. But there's not, you know, it's still new, right? The governance and the processes around AI and healthcare still leave a lot of open, open questions.
So how can you prepare? Industry leaders are instructing organizations, both providers and non providers to focus on a few different strategies to really navigate this. So we are looking at cost capital and scenario planning, cost and efficiency. We're seeing looking at revenue loss mitigation and workforce and access management. So Alex, which bucket would you say LVHN is most concerned about and what are you doing to prepare? Great question. So I, I look at this slide and look at those 4 buckets on the left hand side and there's a reason why I have that top left one that capital, capital and scenario planning.
I really do consider that to be probably the most challenge that we have. The remaining 3 here are the the mitigators and and the items that we work on a daily basis. All, all leaders everywhere across the healthcare industry working on cost containment and efficiency, revenue loss mitigation strategy and that workforce access management and focusing on those to help create capital dollars for scenario planning. I think every year our capital budget goes lower and lower and tighter and tighter. We strap our belts to figure out where we can get the capital and invest in new technology. I think one of the things that we have to work on are the financial pressures and reimbursement challenges.
Working on the inflation and the rising costs and declining reimbursements, as I said before, but also working on technological integration and that data overload while new surgical strategies and technologies are. Becoming more active and analytical. Analytical tools are offering many, many promises. Many systems are still struggling with implementing them, interoperability and training and leading to inefficiency and underutilization of these great programs. But at the same time, we're still recruiting new surgeons, new procedures, new technology, new instrumentation. That's all capital. And I think we all struggle with, well, how can we get more capital dollars if we're investing in all of this?
But you need to work on these tools to help you mitigate all of these so you do have those capital dollars. So I think that's very, very important. I know you probably would have also said all four in this scenario too, but I want to focus on the bottom left, which is how are you reframing things in that cost, containment and efficiency bucket to make sure you're not reverting to the same old tactics that may have worked across the past decade. It is all about active management and I know that's a terminology most people are aware of, but really holding people accountable and active management moving forward and being predictive in your decision making and utilizing the software and the AII.
Don't want to tease everything, but we'll talk about it. But really moving away from historical reporting and getting to active management data processing. Yeah, well, you're right. Let's not tease at all. But more importantly, let's get away from this doom and gloom that everyone's already probably pretty intimately familiar with and talk about how we can go from challenges to change. So when approaching change management, organizations need to have a multi pronged approach. Today we're going to narrow in on 2 procedure, cost, variation and increasing OR capacity. We're going to cover some best practices in real world examples in the following slides.
But in both prongs, organizations need to shift their approach. Looking backwards for ways to improve is just not viable. Without real time visibility and standardization, organizations are going to risk overspending and underperforming for cost reduction. Transparency is key. We need to empower surgeons with comprehensive data in the moment to avoid unnecessary use from a capacity and profitability lens. Ineffective site of care decisions, ineffective block utilization and poor throughput are leading to a backlog, all of which can restrict revenue potential. So active and predictive data is the big change here. How can we predict time that will be underutilized and then proactively fill those slots?
So Alex will share some best practices, but I want to thank the group will find even more interesting is his real world application. And so, Alex, I'd love for you to share how you and your organization are evolving your approach for these challenges. So first, let me just tell you a little about Lehigh Valley Health Network. In our region that's part of Jefferson Health. So if you think of Lehigh Valley, we're located out in the Allentown area and our region goes from Allentown all the way out to north of Scranton in Northeast Pennsylvania and even out to the West in our school region.
We have a Level 1 trauma center in Allentown known in Cedar Crest. And a Level 2 trauma center, actually multiple level 2 trauma centers. We encompass about 105 operating rooms across these hospitals. It's 9 hospitals, 14 surgical locations. We do about 105,000 surgical procedures. When we add our procedural level which is our endoscopy we we get around 180 a 190,000 then with. Procedures. We are A1 to 11. That's a circulator, a scrub tech and CRNA in the room.
We are struggling, I say with scrub techs because we are our filler. Schools are closing around the neighborhood so we are using LPN staff and some RNS to function as a scrub. And we are about 98% employed as physicians. So our we have a very robust surgical group and they are part of our Lehigh Valley physician group practice. But in today's discussion, we're really going to focus on the southern part of our Lehigh region. We call it our 22 corridor. So imagine, really just so you have it in mind, a highway that runs east to West about 25 miles with seven hospitals on it.
And we have some multiple things that we'll discuss, but just think of that as the geographical, geographical region that we'll discuss during today. Good. And let's start on that surgical supply cost reduction prong. And so industry recommendations are cost containment and efficiency are not necessarily novel, right? Remove variation, optimize day of surgery efficiency. But what is new is how we can incorporate new data and new technology to push the needle further when tackling cost reduction. Leaders really need to be asking themselves some of these questions on the screen, no?
Which workflows are contributing most to our overtime or our first case delays? What are the root causes of scheduling conflicts? What can AI in real time analytics and how can they be leveraged to identify inefficiencies and Dr. immediate improvements? And also beyond just asking for those questions need to be collecting this data that you see on the right. You need to have this granular level of visibility into performance at the site at the provider level all the way down to even rooms. And that's teasing our second section here. But having all this data and asking your questions.
So what do we really suggest that you do? And I'm actually going to start on the right hand side of that screen. So to be truly successful, we need to have all that data together and that is the hard part. So looking at reimbursement and financial class, overall cost, profiles of supplies and direct cost and the quality outcomes, emphasize quality outcomes. Here are what we need to help make decisions on where a total knee should be done. And we need to be leveraging tools like Crimson AIä to help forecast the patient trends. See if your Medicaid patient population has always been a high chunk of your volume.
Assess your payer mix. Right, and I know I skipped straight to the data, but paralysis by data analysis is a real thing. So don't boil the ocean, you know, target high impact opportunities. And the other thing I'll recommend is that small drops do add up over time. And more important than just that growing savings bucket is that it really helps with surgeon buy in. So small changes with big outcomes get all stakeholders excited by the potential. And this is where Alex has a lot of great things to add here.
Thanks, Laura. Nine years ago when we started this adventure, we, we were definitely some skeptics when we started with Laura and team. And I can't thank her enough for the, for the, the steps because we were definitely one of the people who were going to boil the ocean. And we, I think all of us do struggle with all the data that's out there. I mean the, the Emrs, your, your epics, your Cerner, your, your meta techs, everything that's out there, there's, there's so much data in there and it, it, it. Becomes difficult to analyze and and put it together, vet the data and then have your surgeons and even other teams trust it.
So definitely taking small steps in the beginning and creating some culture. Really will help you assemble this and even then move forward and we'll talk about it now on this slide. We're going to take this slide and really start from the bottom up. So looking at when we started in our FY16. You'll see that cultivating that open culture and and buy in from our surgeons. So it requires a culture, we get that, but it's buy in. And how do we get the buy in? Well, we include our business services team, our operational leadership team, our clinical leads, our surgeons, our department leadership, operational leadership, regular scheduled cadence of meetings with a standing agenda.
We, we suffered a little in the beginning when we tried to adjust the agenda to everybody's wishes, but found out if you stick to a standing agenda with the primary points, you achieve much more fruition on on the things that you want to achieve. So including your operational efficiencies, your cost, you utilization, value analysis, procedural variation and then support that with that next by building the transparency with with the tool which is Crimson AIä in our case. So support with accurate and vetted data come out with the visuals to the surgeons, put them in the room. Let them try to pick at it, create some friction at least to say, hey, tell me where I'm wrong and if I if I am wrong, let's fix it together.
Let us help understand each other and where we're coming from. So we got to the point where we worked with these surgeons to ensure that they're so comfortable with this data, they're actually speaking to it and they're the ones now reporting it to their division chiefs leadership, our surge exec, our operational leaders. They've gotten so comfortable now where they can speak to it. They walk into the operating room and they see something on the back table, don't open that. It's like the first thing that comes out of the mouth.
They know that the cost variation, that procedural variation occurs with just opening one simple item on that table. So sharing that has really helped build the confidence not just for the operational team, but really for the surgeons and them feeling comfortable having difficult conversations. Next, strengthening the vendor partnerships. It's not always about price parity and getting the best price. Yes, that's one of the items we always need the best dollar. But having that risk relationship with your with with your software company, I mean, I mean Crimson AIä really took the risk with us to understand what things we needed to do moving forward.
And then we've built relationships with other vendors in the industry. And I, I think it's, it's very important that when we share the information, yes, it's, it's confidential and we don't share all the pricing and everything, but we do get to say, hey, you cost more and this and our reimbursement we're noting is not covering your supply costs. What can we do to help mitigate that? And at the same time, we're looking at vendors who are committed to bring the value based care and patient quality. It's not always just about the product. We're we're going to partner with people who care about what they're doing.
So I think that's very, very important. The next second to last year is you're developing your focus factories. This is your site of care work. So I talked about that geography, that 25 mile stretch of highway in the seven hospitals. So imagine this, we have 4 hospitals that are performing orthopedics. Three of those four are performing spine, 2 perform ophthalmology, five of them are performing GYN and six of those seven are performing general surgery. So that boggled us. I mean, we realized, man, we, we really have some side of care work that we need to do because we're duplicating expenses, triplicating, quadrupling, whatever you want to say across these these areas.
So we have to focus on geographics market share, where are we competing, where do we know patients will travel? And providing that focus factory the best excellence of care for that specific service line are key metrics. It's not always about the price, but it's also about the quality. So we really, really worked on that and are doing great work and strides on that. And then last but not least, this final probably about 18 months is moving away from historic data. We don't want to take the fire hose out anymore and just burn out the fires. We really need to start predicting when the fires are going to occur and why they are.
Going to occur. So it's continuous data. Capture. We all know we struggle with the vast amounts of data mining and across all of the perioperative continuum. I mean, I mean, I'll say I'm probably a little egocentric on periop services, but I will say we're probably one of the biggest divisions with so much ancillary touches. We talk about preoperative assessments, intraoperative events, postoperative outcomes. Our active data management is what is the future and ensures that the data is captured in real time and rather than being retrospective. So real time integration, we provide situational awareness with integrating our data with our EHR.
We're monitoring our devices real time. I kid you not, when I get that seven O 2, seven O 5:00 AM phone call, what are we doing? What's the change, what course directions we have to take to to mitigate any loss in volume or if we had call outs, staff shortages. It's it's a daily, a daily task. But with this, with this active management and the AI and the predictive analysis, we're gaining trust and we have data stewardship. We're maintaining high quality, secure and reliable data. And the active data management really supports this by enforcing our standards and really holding everybody accountable.
There's no way to hide from the numbers. They tell us every day what we should be doing next. So it's very, very important. Yeah, I think these stories highlight that even further. Thanks. Laura always loves highlighting this one. It's rather old because now I think about it, my God, we're going to be starting a new perioperative Winter Olympics because we're going into the Winter Olympics. But last Winter Olympics we did a perioperative Olympics and it was really actually a very fun task. We use the old scoring of a artistic score, which is the creativity of the idea and a technical score for financial savings.
And we brought up Crimson AIä to help us as the staff members came to us. We just opened up our laptops and took some of the ideas and, and, and that alone in the six months that we did, that was perioperative Olympics. I kid you not, it was realized savings of over $900,000. And then what that did was actually turned to the non believers, actually into believers and even empower the frontline staff to say, Hey, actually what I said matters. I mean, it wasn't cost avoidance. This was realized savings reduce the pars and we, we noticed we, the waste that goes on in the operating room is unimaginable.
And now it's just moved into a quarterly active management, a service line data. So now because we've gotten ahead of it, we, we only have to report out on a quarterly and say, hey, the variance opportunity that we had last month was only $300,000. And that was probably due to some constructs and orthopedics and some usage of different vendors. And lastly, but definitely not least because we had to keep it going, we did a Super Bowl of savings. And this one always makes Laura laugh too, because someone came to me with the idea of water and water savings.
And I'm like, what are you talking about? And they, they took me to the OR and I stood in the corner and I realized the scrub sinks didn't have sensors on it. And between the scrub tech, the surgeon, the circulators or whoever was scrubbing into the room were using the water. And they would kick the plate and wait for the water to warm up. And that weekend I learned how much water flowed by liter per minute through the scrub sink. But it was a $980,000 water bill savings just by installing the sensors and going in there and measuring it. You wouldn't think that, but something very creative and and just really, really great work, which makes me proud of not only the work that we've done with Optum, but of the work that our frontline staff are doing on a daily basis.
That's definitely the emphasis and going back to the kind of the small buck, small drops in the bucket add up to huge numbers. And the people who are there day in and day out are seeing the greatest opportunity. And we just need to tap into that and leverage their voices. So you heard those two stories, but your your overall story is pretty remarkable too, Alex. Thanks, Laura. And it's true, Laura says. I mean, a lot of people say, oh, the 24,000 savings not going to help the 24,000.
Trust me, at 24,000, multiply it by 12, all you need is 12 of them. That's, that's a quarter million there. It's, it's, it's a lot of great work. And I, I can't believe it because I, I actually had to do the math over 9 years. It is. And I, it's not cost avoidance. It's $27 million in realized cost savings and it is, it is an effort on everyone. But moving into the AI technology where we can see where we're going to see potential loss, we get ahead of it.
And as the slide says an 8 to one on ROI and you'll see the big jump and everybody says, well, COVID Alex hurt us all. Yes, it did, but it's also an opportunity. It made us realize what we had to do on the supply chain side and the work that. Goes in there. Because we know costs are going to go up, but that again goes to goes to making sure you're making partnerships. With the. Right. Vendors, the ones that do want to partner with you and you'll see this just great work that's happened over the nine years.
I will say that last little blip where you see the line go down, we did have some change as we merged with Jefferson. So we had a team reorganization as we were trying to merge our teams together. So a lot of work was done as we changed our ERP to work day. So I know everybody will say, well, look what you did in 2025, just know that we've doubled in size. So I expect that to also triple in size and say things in our coming years as we are now 1 Jefferson Health. Well, I just find these stories remarkable and and it's a showcase of every possible way that you can try and drive down costs.
But in the interest of time, let's shift to our capacity prong and your instance which is around rooms running. And so when we think about capacity, it is a little bit more complex of a challenge to solve for because you actually need to have the patient demand and you need to have the staff to work those cases. And yes, capital investment is required to support different services, locations, etcetera. So there are a lot of questions you need to ask yourself, you know, very detailed there in the center, you know what is your staff allocation, what are barriers to cross training staff, what are our projected surgical volumes for the next one to three years?
How do they currently align with our current capacity trends and our plan for the future And also a lot of data and different data sources that can inform that strategic decision making. So you heard us talk about that before. Yes, utilization and day of surgery efficiency are definitely ones to help you understand what you physically can support. But adding in that financial profile is pretty important too as you're making strategic decisions on site of care or a block allocations, whether you do that at an individual surgeon holder level, a group block, or even a service block. So you want to be looking at all this data combined together.
But ultimately, we really just recommend focusing on flexible staffing models and Alex gets that streamline scheduling and site of care optimization. So all of this really require establishing a stronger governance. That's the underlying layer here, a stronger governance with better data. So Alex, why don't you tell us a little bit more around how you were tackling this challenge? Absolutely. What you're looking at, I call it the ski slope. It's, it's our weekend rooms running and we try to run at our level 1 trauma center, 3 operating rooms about 8 to 10 hours.
And then we have our call teams come in for the remaining 2 rooms for the off hours. But I think we all struggle and we still probably continue to struggle post COVID with temporary labor. And depending on your geographic area, temporary labor has been probably the true expense that's been hindering us on our capital requests and so forth because we're. Having to pay temporary labor to ensure that we have a workforce in our operating room. So we came to the conclusion that hey, to save money, we looked at creating our own temporary labor force, or what we actually call our internal float pool. So on the weekend we took this study and what you're looking at is this, this slide of hours running and then the room's in half hour and then we drill down then into the service lines.
So we dedicate a room to general general surgery. Those are in your Gray and we dedicated a room to orthopedics. But we knew anecdotally that we had urology, Pediatrics, transplant, neurosurgery and a number of other service lines fighting for that third room constantly, especially on the weekend. So with Crimson AI'sä help, we were able to then indicate the percent hours versus the percent of volume in those three rooms. So obviously it it, it's very understandable that general and orthopedics had a pretty proportional lower to volume as well as our Pediatrics urology. But while transplant and neurosurgery had lower volume, they had higher percent volume in hours.
Obviously because they're longer cases, higher acuity take longer in the room, which indicates us while it was happening. Frequently, we probably weren't managing the resources accurately enough to manage the transplant in neuro, which let us believe that we definitely needed to create an incentive call team for our neurosurgery and transplant. Additionally, we did the same thing for our just regular daytime operating rooms between those seven locations that I spoke to you previously about in that geographic 25 mile highway. And the same thing we there we did there was with this data, we were able to determine 8 float or temporary labor that would float between these seven locations. And by doing that I'll let Laura go to the next slide because that's the hit.
It saves $1.3 million in about 6 months. And this is the difference between the temporary labor and yes I'm not, I'm not going to sugarcoat it. We do pay these float pool a higher incentive rate, but it is still a 7 digit savings. It also saved 4.214 days of length of stay at just our. Level 1 trauma center and it allow us to reach our labor budget almost by 95%. Because I think all of us struggle on the day-to-day call to say, Hey, what are you doing about reducing your temp labor expenses? What, what tools are we utilizing?
So it's just more than block utilization. It's more than it's everybody being efficient in the OR and the turnover. It's utilizing AI technology to really. Focus on what are the service lines that we need to have maybe a special workforce for. What are the service lines that we need to reduce throughput IE orthopedics in general? The last thing we need is a a broken arm sitting in the hospital for three days because we have. Level 2, Level 3 femur fractures coming through. So the work done here through this AI technology has just been fantastic, especially these last few months as we continue to work through some of our temp labor challenges that we have.
And it's pretty remarkable and what I think is actually really great about LBHN success in both stories and really any similar story of a Crimson AIä client is it follows A replicable workflow. So whether through the technology itself, through your expert advisor team that comes along with your technology membership, we're proactively pushing organizations to where the opportunities lie. And I, I want to stress that because that's the hardest part, is where do you decide where am I kind of going to get the best bang for my buck? We're making sure those are the first things that you're seeing.
So you're really deploying your limited time and resources effectively. But yeah, so proactively pushing the opportunities, but then the breadth and depth of the data that's at our fingertips really expedite root cause analysis. The introduction of AI will eliminate the need for further data mining and manipulation. And so in one click you can have an AI assisted recommendation for an intervention. So we recommend you substitute this item for this. We recommend you make a preference card quantity update. You know, instead of opening two shift, one to hold and one to open and then you know, the other part, we focused on the supplies.
But this is just as much of an important factor here is we are able to then link all of our analysis with inpatient and ambulatory quality data and quality measures to ensure that quality of care is never compromised. And this builds a lot of confidence with your surgeon leaders because you're showing them we're asking to make this change. We're very cognizant that patient, patient care comes first. And here's some data to help you feel confident in this change. And then lastly, you know, we implement and we monitor the success of that intervention. We want to make sure there's no slippage.
And that's kind of how you get to those huge, you know, almost $30 million savings like Lehigh Valley. And Alex has touched on this throughout the presentation. But in order to successfully navigate a lot of these challenges, your data needs to be forward-looking. You need that active data management and so long gone are the days where you're acting on historical trending to achieve the results your organization's need. You know that left hand side of the slide the past. You really need to be looking at real time data to be fluid enough to act in the moment. Swap out a supply before opening it.
Reassign a room on day of you know for optimal throughput and time management. Leverage the future schedule to make decisions right within your work flows. And then on this future part, you know, leveraging predictive analytics to solve the problems before it ever becomes 1. And that's where Crimson AIä can really help you do just that. So before we give you a little bit more detail on all the things that are Crimson AIä, we do have one more poll and this is around your data strategy. And so where would you say or sorry, which would you say best describes where your organization stands on its data strategy that it's still relying on historical data and past trends, that you're starting to use more real time data, but everything's still pretty reactive or option number C that you're already in this predictive analytics and forward-looking space to proact proactively shape the strategy.
So we'll give a minute here for folks to submit their thoughts and their results before we see where people stand. And what I like about this poll and why we wanted to make one around this question is I would think that most organizations think they are between B&C or that's where they there are, they've made some investments to be operating in that space. But when push comes to shove and the reality of the data and where, how and where you're interacting with it, you're still pretty operating to some traditional tactics that we've done in the past. I think we're.
Getting there, Laura, though. I hope so. I hope so too. All right, I'm seeing a little bit of a lull, so let's just and I'm keeping an eye on the clock here, so let's actually ship. So here we go. It's basically 5050 and but 5050 on past and then shifting into more real time. So not a surprise here at least, you know, Alex, for you and I and kind of our experience working with folks like you and you being on the front lines there.
OK, So without further ado, in our last kind of 5 minutes here, we talked about Crimson AIä. So let's actually explain all that comes with Crimson AIä. So it is a reimagining of some of our legacy solutions that came to Optum as part of that Advisory Board acquisition solutions like surgical profitability Compass. There's also Crimson Continuum of Care, which was once a market leader in our hospital quality and patient reporting space for almost 20 years. But we've taken insights from those legacy products and heavily invested in revamping and relaunching them, and we focused on modularization. So our goal as Optim is to help organizations, you know, hospitals and health systems more easily work with us through a single unified platform.
And then we'll enable different experiences depending on what you as a client need. So there are 7 modules either available today or being released across this year on the screen. And but I'm going to touch on the two that Alex has spoken to to support Lehigh, the surgical cost and surgical capacity modules. Surgical cost is addressing the care variation reduction and supply optimization. It offers a very fast visibility into cost drivers, potential alternatives and performance across all the different surgical supply cost drivers that your organization directly linking in that quality component. And then surgical capacity addresses schedule management and utilization.
It offers dynamic data-driven scheduling systems that adjust in real time based on his both historical procedure data but also patient demand in the future schedule. And wrapped around all of that right is surgeon specific data and patient complexity and so tiny on the screen here, but some visuals to kind of see at least on the right hand side, you can see some AI recommended block adjustment changes. And a primary differentiator for us and Crimson AIä is that investment in the AI. So there are predictive analytics, there is an AI chat feature, there is smart opportunities. And those smart opportunities address that most challenging part of analytics, which is taking in all the data, aggregating it accurately, and then mining it to see what you should work on.
And so we're really leaning on AI to do that data mining and processing portion. So I know people can AI can feel like the Wild West right now, but Optum has very strict AI governance. This has nothing to do with patient care decisions. We are just focusing on our AI for speed to insights. So there are guardrails that are included. So you won't ever see a recommended intervention or suggestion that you wouldn't naturally see or work on with our advisor team today. And you can see the results that this type of data fuels.
So Alex has achieved the big ones, you know 27,000,000, but on average each year our client sees about $5,000,000 in annual growth in revenue associated with improving your prime time hours from a capacity management perspective and roughly a half $1,000,000 in that true realized cost savings that are easily measurable and seen in the bottom line. And so at this point we are wrapping up, we'll open up some Q&A. But you know the big things to really take away here are that the pressures are only mounting and getting worse. There's the perioperative leaders, there's multiple approaches you can take, but two that will feel really manageable are around the capacity planning and management and cost reduction.
The emphasis in both situations is having transparency into data, complex data, forward-looking data that active data management and tools like Crimson AIä can be that data engine to support all those conversations and initiatives. So with that, I will turn it back to you, Jay, to see if we haven't had any questions come through. Thank you again to Laura and Alex for a great presentation. This now brings us to the Q and a portion of the program. Again, you may submit questions to the Q and a box in the lower left of the screen.
And Please note that all questions will remain anonymous. We have a question here asking about overstaffing and this person is asking, do you have a preferred info source for benchmarking staffing levels for each service line? Laura, I'll throw this to you first. I'll actually throw it to Alex I. Was always going to say I would have to phone a friend but it is dependent on service line. I do agree the neurosurgery and cardiothoracic service lines usually tend to have the RN and the scrub function as well as the circulators function. In our robotic platforms, we are having had the bedside assist in addition then to the circulator and surgeon at the room.
So it, it is really it is definitely service line specific and we have to focus. I'll have to get back to you. I mean, I'm glad offline if, if they want to go through Jay to get that answer. But like I said, it is service line specific. We don't it, it really does depend on the state and the regulations that are behind that for your, your DoH, right? Another question we have is if if you remove the 90% plus employment model, employed model, would you, would your approach still hold and would you still see the same results?
Absolutely, absolutely. As I mentioned, probably in the slide deck when I said bottom up, you got to build the culture. It doesn't matter if the physicians are employed or not. If you get them at the table and you do the work you'll have to do is get them at the table that once you get them to the table and show them the data and show them what those differences are in procedural variation. And what that has is a downstream effect of its supply expense reducing your reimbursement and margin and, and show that and work with them to show what their peers are doing.
You can build that culture and you literally will get to the culture where then they'll be speaking to it and they're in the room explaining it to you and it makes your job a little easier on some days. Not going to say they. Don't complain a lot, yeah. You'll still get complaints, but surgeons are inherently competitive and they are hungry. They're learners, they're hungry for information. And so usually once you start putting this level of visibility, even if it's just for their own, they want to be cheaper. They know that these costs pass through to their patients.
They want to have, you know, that optimal, best quality, lowest possible care. So once you see it, they're going to be knocking down your door to ask for a lot of questions on what does this cost compared to that and could I switch? You know, that's a good question. Great. Another question someone asks, can you speak more to the design of the multi specialty float pool such as eligibility, cross training and expected savings for FTE? Absolutely. When we designed the the flow pool, obviously one of the concerns was we had to ensure that the people volunteering for this flow pool were in critical acuity service lines and that they could do more than 5 service lines and be fluent in those service lines.
So a great deal of work was done to interview to ensure their capability and skill set was valid and and vetted and we created that the savings was 125,000 per FTE. That's your difference between the temp labor and the increased incentive. So when you multiply that, it's a great number. So like I said, 10 travelers, which was about our number generates $1.3 million in savings. Another question we have is when standard, when standardizing supplies, which clinical outcomes do you show surgeons to validate safety and efficacy trade-offs? I'm happy to take this one.
So Crimson AIä has over 1000 and growing quality measures that can be associated. So the answer here is actually what is most meaningful to that surgeon or that specific surgical specialty, right? We ideally we can get, get down to specialty specific measures, but it is entirely customized. So you can start off with some of the big 4, you know, what is your readmission rate, what are your complication rates, surgical site infection rates, mortality, you know, those are pretty universal no matter which type of procedure you're doing. Or you can get more granular and focus on specific hacks or you know, within CD or ortho, there are some more specific different measures associated with the procedures.
They're doing great. And another person asks, do you use Crimson AIä with Epic and or is it integrated? We'll start, but I'd love Alex, your take. So yes, we do use it with Epic. In fact, I would say about 60% of the Crimson AIä cohort is on Epic. And so it, we do have a feedback loop for certain parts of and feature functionality in which we can push things back into the EMR. But for majority of the time you're actually using them side by side. And that's because it's, you know, once again, speed to insights, surgeon friendly visuals to help drive the conversation, which might not be as easy to achieve in a in an EHR.
But Alex. Yeah, absolutely. The, the, as I mentioned before, I think the EHR well, well a fantastic tool to move patients around. It's still sluggish where I say it's a warehouse of data. They're getting better. All the EH Rs are trying, but I think we all agree that EH Rs were built to help patients move through the, the, the hospital care, we'll call it, but it's tools such as as Crimson AIä and, and, and I mean, that's why there's so many vendors on the market, we'll say that are investing their time to help operational leaders and, and, and folks like us to come up with better visualizations, utilize AI predictive analytics to find the potholes in the road that are going to come up.
So yes, they are using in in conjunction. The HR is feeding the data, but it's it's really the the the software that's giving you the the results. And staying on the topic of AI, someone asked what AI guardrails are in place so clinicians trust recommendations from smart opportunities. Yeah. So I I'd write if you do have deep questions, I have a kind of a full novel to send your way. But so all of our AI is trained on a de identified database that has over 51 million clinical and claims lives.
And so all of the model training and testing that we're doing, we're actually doing it in a pretty granular level. So it needs to pass the percentage standards on that at a higher level, but we need to slice that by race, by gender, by socioeconomic, ethnicity, ethnicity. You know, we're really drilling down for in a service on a procedure down to that level to guarantee that there's no bias involved with any of our risk adjustment methodology or any of our other AI generated recommendations. We also partner with our clinical and industry leaders with an Optum. So one part of its data, the other part is industry best practice that is funneled into these AI models to bring forward some of these recommendations.
I love to hear that answer because Laura knows my, my dissertation for my doctorate was the lack of governance in AI is specifically with the HR records. And it's, it's actually a phenomenal study and a little scary when you start doing the reading on how, how there is such a lack of governance on, on the state level and even governmental level, federal level. And it's been left actually to, to the hospitals and to organizations such as Optum to ensure the safety and the guardrails are put in place and that they were appropriate. And I'm, I'm very proud and joining with Jefferson Health and working with Austin that we've put those guardrails up and it's, we have an AI council that meets monthly to review that we are doing the appropriate things and that those guardrails exist.
So it's very important to on both sides, on the software companies and the healthcare industry to ensure that we're doing the right thing for our patients and not utilizing AI for negative impact. And someone asked what process can we use to reconcile the difference between scheduled case length and actual operative time to improve block utilization and scheduling accuracy? Would this also be Crimson AIä 100%? It's a very simple report that we can put in place and actually something we really recommend using as you're putting together your blocks and, and block time. So it's one of many different factors we recommend bringing forward.
It's a great tool in that aspect. It's it's learning from your system and getting better accuracy. So a great, great tool. Yeah, finding that with scheduling lead time is another metric that intersects with that right one. Are you scheduling the right amount of time too much, too little. But then as we think about trying to create capacity, how far in advance, you know, do we need to be freeing up time to get some of these cases brought in and onto the schedule? I think we have time to sneak in one more question before we wrap up.
Someone asked what are the most common blind spots all systems have when it comes to or block utilization. That's an interesting one. I would take that question and put it back. Sorry to answer a question with a question, but it depends what your process is. What are you trying to achieve? Who controls the process? Is it inherently bias? And that's the question I I put back because sometimes I, I've seen health organizations where the chairs have control of the block utilization. So there's inherent bias that, oh, well, they're not going to release their group block because they're going to want to make sure that their provider is running it lower the days where we, we have to go.
Well, that's my block. Well, in fact, actually that is the hospital's block. That's not the surgeon's block. That's not not the group's block. It is the hospital block. We are looking to make sure that we are being efficient. If I don't have a surgeon that's on time every day, at least 90% of the time utilizing their blocks, 75% of the time, I'm not going to give them new block or I'm not going to allow them to follow themselves in their own room and add-ons occur because they're not being efficient stewards of the block.
So there are some culture changes that you do have to agree upon. And again, I, I will throw out to Jefferson Health, we, we just went through this as we've merged now 34 hospitals and we are now one scheduling policy that will be up and live April with these guidelines and use of them. So the pit holes are who's managing it, how are we releasing, what are the marketplace releases, how are releasing them? What are those metrics, What are the percent utilization? Those are the pitfalls, because if you don't make them standardized and you don't abide by them, you'll never achieve the block utilization you want to achieve.
Yeah. And in addition to that, but you're kind of touched on it, I'm just going to say it even clearer. It's it's the policy. It is what is written into the policy. How aggressive is it and how strict is your enforcement? Because there are plenty of organizations who still say they need to have 3/4 of underperformance before they take up the block away. Well, guess what? That's nine months of leaving gigantic holes in your schedule that are, you know, staff sitting around with no patient because we're a little too timid and to take on some, you know, be a little bit more regressive.
And at what point are we going to enforce these policies? Agreed. Great. That's all the time we have for today. I want to thank Laura Kennedy and Alex Warman once again for an excellent presentation and to our sponsor Optim for making this program possible. Finally, thank you to you and our audience for participating today. We hope you'll join us in the future for another Health Leaders webinar. This concludes today's program.
Thank you. Thank you. Thank you.
