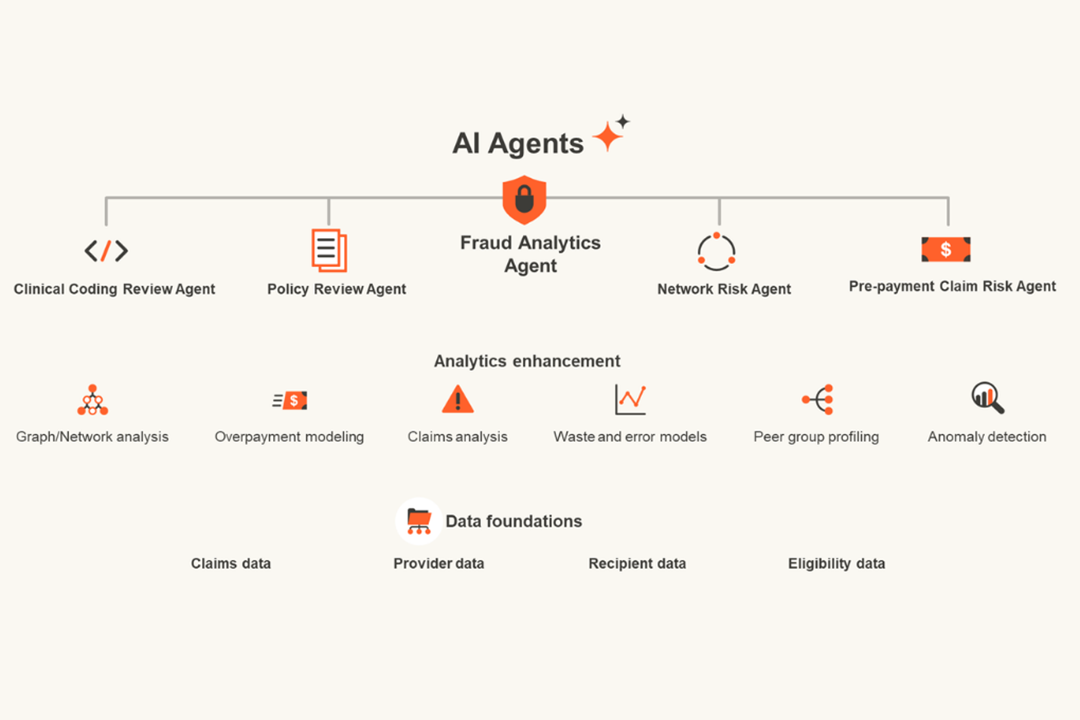
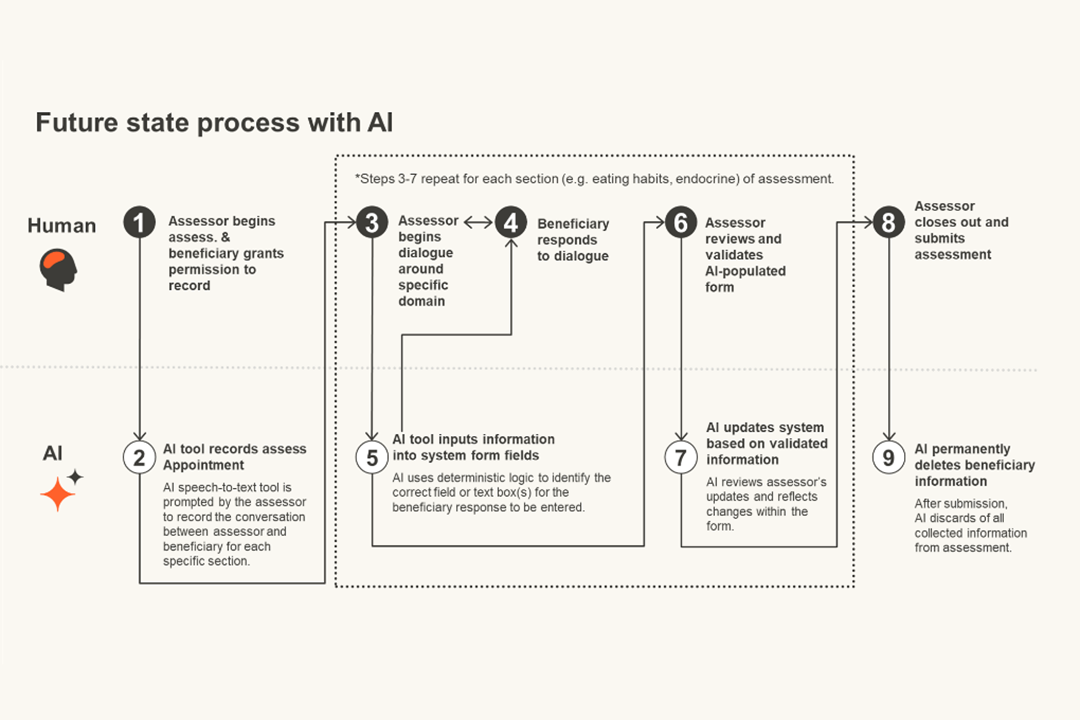
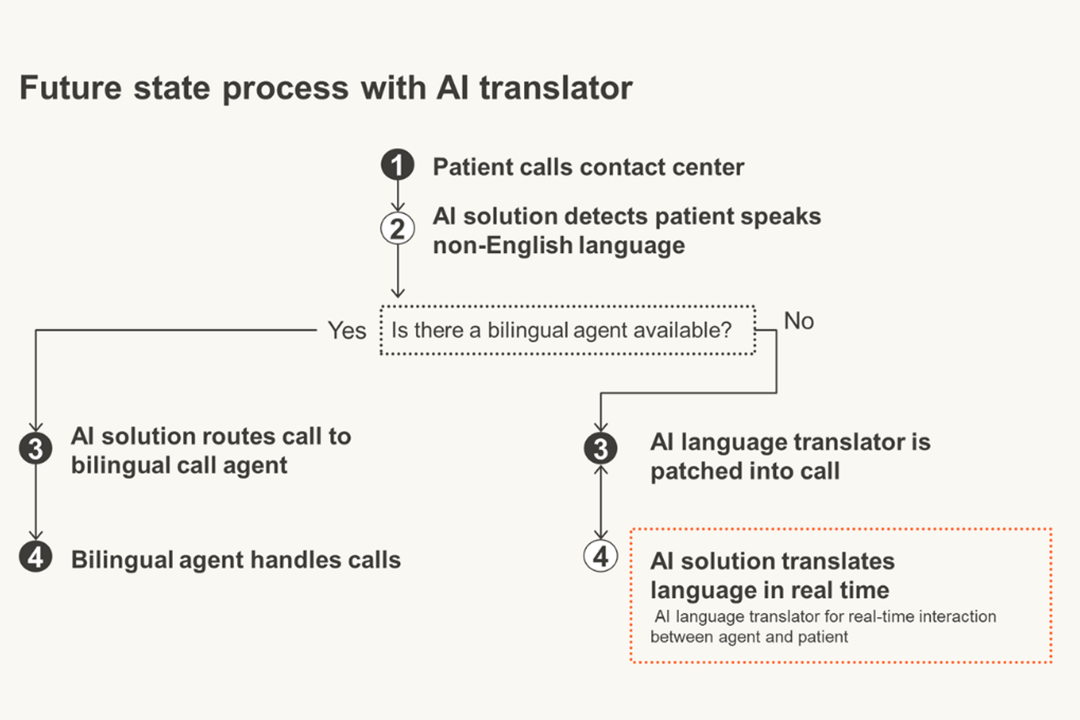
Why does AI matter?
State health programs face a growing set of operational and policy challenges, including:
- Increasing complexity across Medicaid program administration and compliance requirements
- Workforce capacity constraints and rising administrative demands
- Ongoing efforts to advance health equity and improve patient and provider experiences
In response to these challenges, many state health programs are exploring and adopting AI‑enabled tools to help modernize operations and support informed decision‑making.